Tinea Incognito Rhonda Lesniak, PhD©, MA, MS, ARNP, BC
Author Information
Content
History
A 27-year-old male presented with complaints of a rash on the abdomen and lower legs. He states the rash began 3 months ago on his right calf but it has been spreading ever since. He was treated with a high-potency topical steroid cream, fluocinonide, but states the rash worsened and spread after using the cream. He complains that the rash itches profusely. He denies contact with outside allergens, new soap, detergent, or chemical agents. He states he does have one cat in the home. The cat mainly stays in the patient's room. He denies any outside activities.
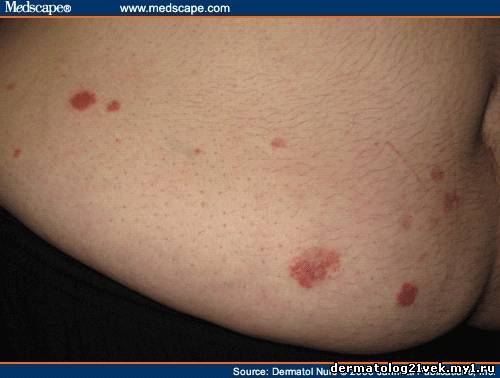

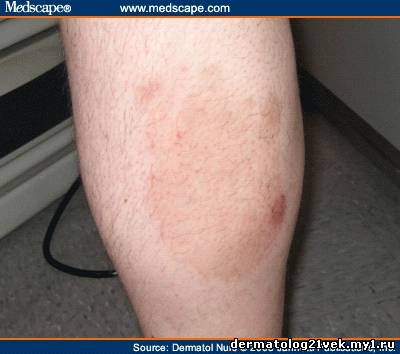
Description
Tinea corporis is a superficial fungal infection involving the body and face, with the exclusion of the beard area in men. The episodes may last for weeks to months and occurs in all age groups. It is more common in tropical or subtropical climates. Tinea incognito occurs if a topical glucocorticoid has been applied and the clinical appearance of the initial tinea lesion is altered, becoming less scaly, more extensive, pustular, pruritic, and painful (Berger, 2007; Committee on Infectious Diseases, American Academy of Pediatrics, 2006; Uphold & Graham, 2003; Wolff, Johnson, & Suurmond, 2005).
Location
Tinea may occur anywhere on the body. Tinea corporis involves the body and face; tinea capitis involves the scalp; tinea pedis involves the foot; tinea cruris involves the groin and upper thighs; tinea unguium involves the nails (onychomycosis).
Etiology
The causative organisms are microsporum (usually from cats), trichophyton (most common cause), and epidermophyton. They are transmitted by direct contact with the infected lesions of humans, animals, or fomites. The fungi may also be transmitted through contact with contaminated surfaces, such as moist, poorly cleaned wrestling mats. The incubation period is not known.
Hallmark of the Disease
The lesions of tinea corporis are annular or circular (hence, the term "ringworm") in shape, and usually well-demarcated and discrete. However, the lesions may converge into a confluent plaque formation, especially if left untreated. The lesions are slightly erythematous with a central, hypopigmented clearing surrounded by a raised, scaly, and sometimes, vesibular border. Pruritus is usually an accompanying symptom. The primary lesions may also be accompanied by a fine, papulovesicular rash on the hands, face, or trunk. This is caused by hypersensitivity to the fungi (Berger, 2007; Committee on Infectious Diseases, American Academy of Pediatrics, 2006; Uphold & Graham, 2003; Wolff, Johnson, & Suurmond, 2005).
Diagnosis
The diagnosis may be confirmed by testing scrapings of the scaly border in a KOH (potassium hydroxide) preparation wet mount. Under microscopic examination, hyphae will be visible.
Treatment
The recommended topical agents are miconazole, clotrimazole, terbinafine, tolnaftate, naftifine, ciclopirox, ketoconazole, econazole, oxiconazole, butenafine, or sulconazole. These agents should be applied once or twice daily for at least 4 weeks and for 1 week after symptoms disappear. If the condition persists, the patient may need a systemic treatment with griseofulvin 250-500 mg bid x 4 to 6 weeks. Alternatives are itraconazole 200 mg qd x 1 week, or terbinafine 250 mg qd x 1 month; however, with these two medications, liver function tests will be necessary as they may be elevated (Berger, 2007; Committee on Infectious Diseases, American Academy of Pediatrics, 2006; Uphold & Graham, 2003; Wolff, Johnson, & Suurmond, 2005).
Normal Course
If left untreated, the disease may extend into the hair follicles, increasing the difficulty of treatment.
Patient Education
Patients should be instructed that tinea is contagious. Good and frequent handwashing should be stressed. Use only lukewarm water and mild soap for bathing or showering. Dry the skin carefully after bathing or perspiring. Drying powder may be used. Keep surfaces (such as wrestling mats) clean and free of moisture and perspiration. Take pets to the veterinarian to check for ringworm as animals may be possible sources of fungal infection.
Nursing Measures
Educate the patient in prevention measures, such as good hygiene and cleaning contaminated areas. Have the household pets checked and treated for infection. Children with tinea corporis may attend school provided the lesion is covered with a bandage.
 Главная
Главная  Tinea Incognito - Форум
Tinea Incognito - Форум Регистрация
Регистрация Вход
Вход
